– FAUSTO GOMEZ OP
One of the great advances of modern medicine is the progressive success of organ transplants. Organ transplantation requires organ donation: for a needy recipient there has to be a generous donor. Unfortunately, there is a great scarcity of human organs for transplant. The limited supply comes mainly from organ donations. It is reported that while the number of transplants done yearly is about 127 thousand, the need of organs for transplantation globally is over two millions. Hence, just about 5 to 6 percent of patients get the organ needed. There are some exceptions, for instance Spain, where 90 per cent of patients needing an organ acquire it (from Observatorio de Bioetica, UCV). By the way, in 2018 the Macau government opened an important website of an organ donation registry.
Grounded on respect for life and identity of the human being, and inspired by the appropriate teaching of Sacred Scriptures and the Magisterium of the Church, we speak of organ transplant and donation (and sale) from an ethical and Christian perspective.
We divide our reflection into three main parts. In the first part, we describe the main terms and distinctions used, and reflect on the issue of deceased donors. In the second part, we focus on living donors and organ recipients. In the third and final section, we consider the recurring ethical issues involved in organ sale. The three parts are published in three issues by O Clarim.
In this first column, we try to answer these questions: What is the nature and what are the kinds of organ transplant and donation? What about transplant of organs from deceased human beings?
1. SIGNIFICANT NOTIONS AND DISTINCTIONS
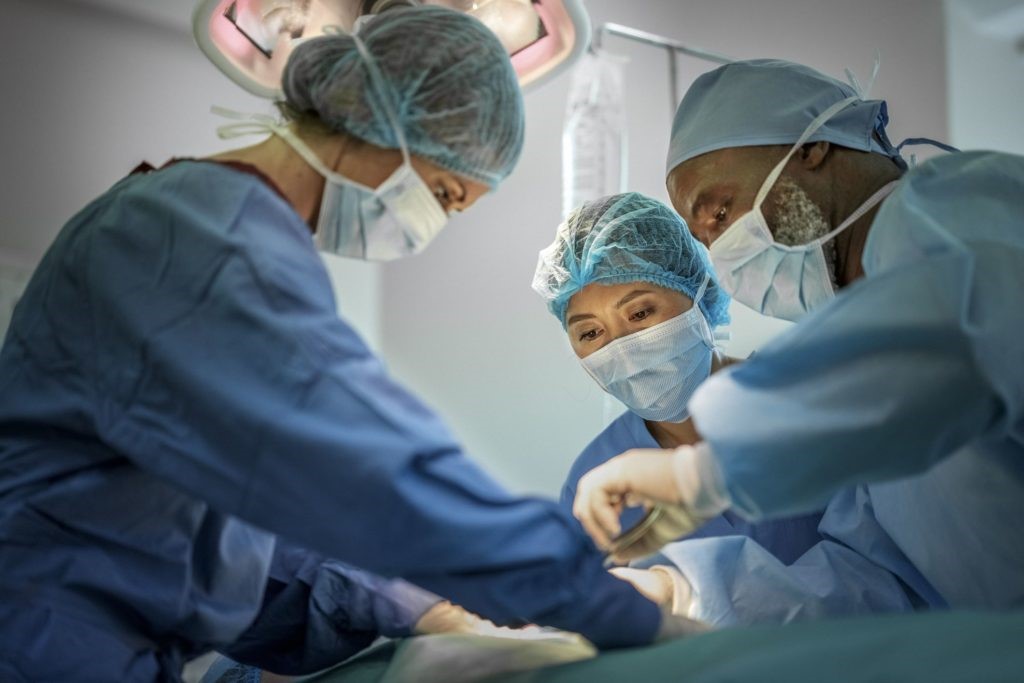
The issues of organ transplant and organ donation are obviously closely interconnected. Organ transplant implies the surgical removal of an organ from a deceased or from a living human being (donor), and its implantation in another living human being (recipient).
There are different kinds of transplants. There is the transfer of a tissue from one part of the body to another part of the body of the same human person (autoplastic or auto graft transplants). There is, moreover, the transplantation of organs from one species to another, from a non-human animal into a human person (heteroplastic or xenograft transplantation, xenotransplantation). Finally, there is the transplantation of organs from a human person to another human person (homoplastic or homograft transplantation). In our reflection, we focus on homoplastic transplants.
Organ donation refers to the free gift of an organ by a human being (in case of deceased donor, by donor, or by family or legitimate representative) to another human being or to an institution (a kidney center, for instance). Organ donation is an act of altruism or of human solidarity. For the Christian in particular, it is an act of charity as love of neighbor or Christian solidarity. Organ donation is a manifestation that the donor not only lives with others but for others.
Organ sale refers to the “exchange” of an organ “for money or its material equivalent.” The source of the organ is the vendor or seller. Strict sale of own human organs appears as commercialization of the body or of body organs of a human person, who is body-soul.
The donor of organs may be a deceased person or a cadaver donor, or a living person or a living donor. The donor, or the family of the donor or legitimate representative gives consent to removal of organ. There are three kinds of consent: free and informed consent, surrogate or substitute consent, and presumed consent.
May a living person donate his or her organs freely (before death) – organs to be taken after his or her death?
2. DONORS OF ORGANS: DECEASED DONORS
In Macau, as in most countries, the transplant of organs generally refers to deceased organs from a person who may have made “a biological testament” or will to donate his/her vital organs or an organ after his or her death.
The two main ethical issues involved in these cases are: the deceased person is truly dead; there is, from the deceased donor or legitimate others, proper consent for the removal of the donated organ.
The procurement of organs from deceased donors can only begin after the donor has truly died. Hence, before the removal of any organ may take place, the diagnosis of death ought to be given. To remove an organ from a cadaver is legitimate after “a sure diagnosis of the donor’s death” (Pius XII).
Scientifically and medically speaking, death is usually defined as the total and irreversible cessation of cardiopulmonary function, or of the function of the entire brain, including the brain stem. The two criteria for declaring death are, then, the traditional criterion, that is, circulatory-respiratory criteria (the patient’s heart stops beating and he/she no longer breaths) and the recent neurological or “brain death” criterion.
Ethically speaking, the cardiorespiratory criterion offers no major problem. The questions come mainly from science and are solved by science. The clinical signs of death are determined by medicine. Good science, moreover, base good ethical guidelines.
Concerning the “brain-death’ criterion, John Paul II affirms (Address, August 29, 2000): “It can be said that the criterion adopted in more recent times for ascertaining the fact of death, namely the complete and irreversible cessation of brain activity, if rigorously applied, does not seem to conflict with the essential elements of a sound anthropology. Therefore a health-worker professionally responsible for ascertaining death can use these criteria in each individual case as the basis for arriving at that degree of assurance in ethical judgment which moral teaching describes as ‘moral certainty.’ This moral certainty is considered necessary and sufficient basis for an ethically correct course of action.”
The Polish Pope adds: Not to respect “objective and adequate criteria which verify the death of the donor in order to increase the availability of organs for transplants” would amount to a form of euthanasia – or murder. If there is no certainly in declaring death through the criteria of “brain death,” then the “principle of precaution must prevail” (Pope Benedict XVI). Certainly, in cases of real doubt, life has preference over death.
Regarding the issue of consent, we ask another ethical question: Is there informed consent from the donor or from his/her surrogate decision-makers? Before his/her death, the capable donor gives explicit free and informed consent for the removal of an organ after his/her death, perhaps through an advance directive or living will, or a donor’s card (in this case, we speak of an opt-in approach). If the patient explicitly expressed refusal to donate the organs no organ may be procured from the body of the deceased person (this is an opt-out approach). The opt-out approach considers everyone a presumed donor, unless the patient, or representative expressed the will not to donate an organ. “Forced donations” (for instance from prisoners) are universally condemned (Bioethicist Bernadette Tobin).
Therefore, when there is no explicit consent for donation or no explicit refusal (non-opposition to donate) by the deceased donor (before death), or the family of the deceased person or a legitimate representative (after death), there is presumed consent. Presumed consent is already lawful in many European countries, and also in Brazil and Singapore. Writes bioethicist James Childress: presumed consent or donation “assumes that the individual (and/or the family) owns and has dispositional authority over cadaver organs, and that the decedent’s prior failure (or the family’s current failure) to dissent constitutes consent.”
With the Catechism of the Catholic Church (CCC, no. 2296), we sum up the teaching of the Church on the matter: “Organ donation after death is a noble and meritorious act and is to be encouraged as an expression of generous solidarity. It is not morally acceptable if the donor or his proxy has not given explicit consent. Moreover, it is not morally admissible directly to bring about the disabling mutilation or death of a human being, even in order to delay the death of other persons.”

 Follow
Follow